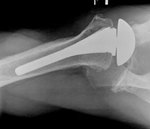
PREOPERATIVE IMAGING & CONSIDERATIONS
- Glenohumeral OA leads to posterior glenoid erosion,
flattening of humeral head.
Rotator cuff tears are uncommon.
- Not recognising posterior wear can lead to glenoid component in retroversion and risk posterior instability.
- CT often useful in preoperative planning and in particular to assess for glenoid version and bone stock.
Major wear of the glenoid may require additional bone graft from the humeral head.
- Before CT,
the glenoid version was measured on axillary radiographs.
- However,
radiographs have been shown ineffective in assessing the glenoid version because of overlapping bones,
variation
in radiographic technique,
and variability and complexity of scapular anatomy.
- Glenoid version = angle between a line drawn from the medial border of the scapula to the center of the glenoid and the line perpendicular to the face of the glenoid on the axial 2D CT slice at or just below the tip of the coracoid
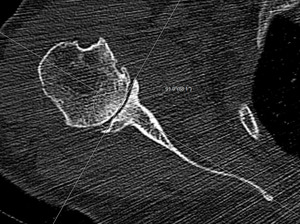
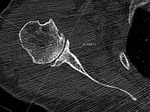
Fig. 4: On axial 2D CT image in bone windows, just below tip of coracoid, line is drawn from medial border of scapula to center of glenoid Line perpendicular to this is drawn. Angle between this line and line perpendicular to face of glenoid is version angle. In this patient, glenoid is retroverted by 2°, which is normal.
- Glenoid: 5o anteversion to 15o retroversion.
- Humeral head: 20-40o retroversion
- In rheumatoid arthritis,
peri-articular erosions and osteopenia.
- Cemented short stemmed prosthesis preferred.
- If glenoid eroded to level of coracoid process,
resurfacing contraindicated.
- Rotator cuff arthropathy - massive tears result in proximal migration of the humeral head.
- Generally,
rotator cuff tears occur in less than 10% of shoulders with OA
- Contraindicated to glenoid resurfacing as it results in eccentric (superior) glenoid loading and early component loosening.
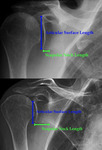
- Scapular neck length (SNL) is important especially in RTSA as a short neck length can predispose to scapular notching.
Studies have shown a SNL of less than 9mm to be significant.
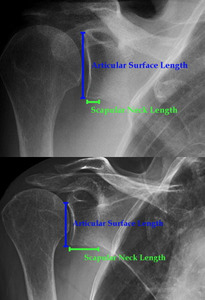
Fig. 34: Radiograph showing short and long scapular neck length.
References: http://www.sciencedirect.com
HEMIARTHROPLASTY
- Humeral head articular surface replaced with a stemmed humeral component or a resurfacing humeral component.
- Stemmed component can be coupled with a standard humeral head Fig. 6 or extended coverage head Fig. 11.
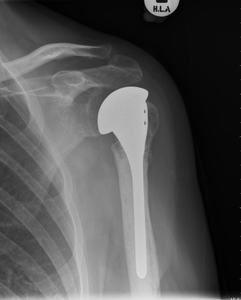
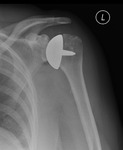
Fig. 6: Cemented hemiarthroplasty with a standard head.
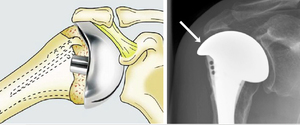
Fig. 11: Implant in glenohumeral arthritis and rotator cuff deficiency. A special prosthesis is used for this surgery that articulates with the undersurface of the arch (white arrow) as well as the glenoid.
References: http://www.orthop.washington.edu/?q=patient-care/shoulder/shoulder-arthritis-cuff-tear-arthropathy-arthroplasty.html
- Prostheses can either be monoblock Fig. 8 or modular Fig. 7.
Stemmed hemiarthroplasty
- Developed over 50 years ago for the treatment of proximal humeral fractures.
Effective in the management of three-part,
four-part and head splitting fractures when stable osteosynthesis is not achievable especially in situations with poor bone quality like severe osteoporosis Fig. 10.
- Used in arthritic conditions where glenoid bone stoke is poor but TSA is superior in primary glenohumeral OA.
- In cuff-tear arthropathy,
TSA can be complicated by glenoid component loosening.
Hemiarthroplasty can provide reasonable results in treatment of glenohumeral arthritis and severe rotator cuff deficiency.
- Cuff-deficient shoulders lead to proximal migration of the humeral head and articulation of the humeral head with the acromion Fig. 17.
- Despite implantation of a standard humeral head,
bone on bone contact between the greater tuberosity and understurface of the acromion can occur.
- This has lead to the development of the Cuff-Tear Arthroplasty (CTA) prosthesis which has an extended humeral articular surface.
In turn this decreases greater tuberosity impingement against the acromion Fig. 11.
- Contraindicated if the coracoacromial ligament is deficient.
Resurfacing hemiarthroplasty Fig. 13
- Effective in a varity of arthritic conditions.
- Replacing humeral head articulating surface with a metal covering or cap Fig. 12.
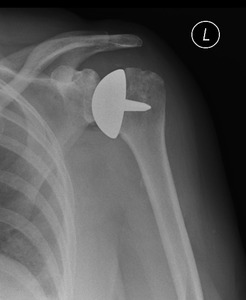
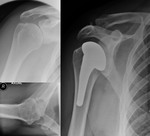
Fig. 12: Resurfacing hemiarthroplasty of the left humeral head.
- Preservation of the humeral head allows the surgeon to maintain the native head-shaft angle,
offset,
inclination,
and version.
- Favoured in younger patients and facilitates future revision to TSA.
TOTAL SHOULDER ARTHROPLASTY
- Most commonly involves stemmed humeral component and a polyethylene glenoid component Fig. 15.
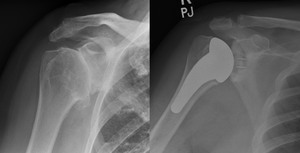
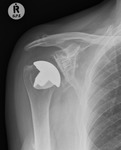
Fig. 15: Right TSA for osteoarthritis. Adequate glenoid bone stock allowed for glenoid fixation. Note the radio-opaque markers within the pegs of the glenoid component.
- Good glenoid bone stock,
and functioning rotator cuff required.
- Can be performed as a resurfacing or stemless TSA Fig. 16.
- TSA with biologic glenoid resurfacing - young patient with disabling arthritis and the manual laborer.
Biologic glenoid resurfacing can be performed with anterior capsule or autologous fascia lata.
REVERSE TOTAL SHOULDER ARTHROPLASTY Fig. 17
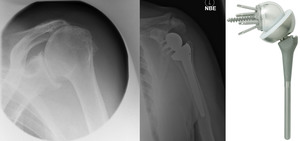
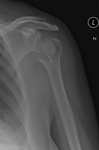
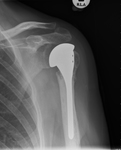
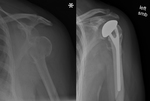
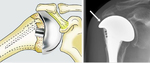
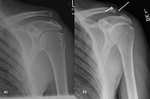
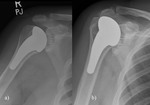
Fig. 17: Reverse TSA. Use of a convex glenoid (hemispheric ball) and concave humerus (articulating cup) to reconstruct the glenohumeral joint. Preoperative images show a severely degenerative cuff tear arthropathy.
- Glenohumeral arthritis combined with severe rotator cuff deficiency
- Centre of rotation moved medially and inferiorly thus placing the deltoid at a mechanical advantage.
Deltoid must therefore be functional.
- More inherent stability and prevents proximal migration of humeral head.
- RTSA difficult to revise - little glenoid bone stock once component is removed.
COMPLICATIONS
Instability
- Excess component retroversion/ anteversion
- Head to small or too inferior (post fracture)
- Subscapular rupture Fig. 37
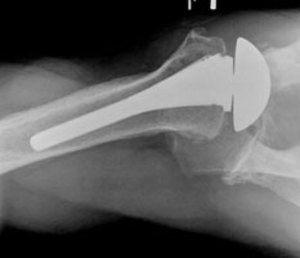
Fig. 37: Axillary view demonstrating anterior subluxation in a TSA with subscapularis deficiency
References: http://www.healio.com
Rotator Cuff Tear Fig. 20
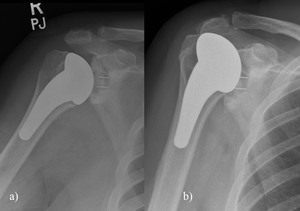
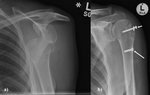
Fig. 20: A) Right TSA performed for OA. b) Proximal migration of the humeral head consistent with rotator cuff dysfunction/ tear.
- Results in superior migration of humerus and glenoid loosening
- This may warrent revision surgery to a RTSA.
Glenoid wear & loosening Fig. 22
- Glenoid bony wear in hemiarthroplasty.
Patient complains of pain.
Radiographic changes increases glenoid sclerosis Fig. 24.
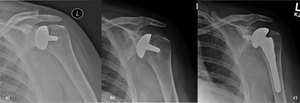
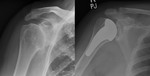
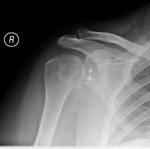
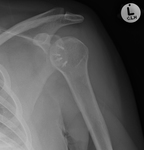
Fig. 24: a) Left Copeland resurfacing hemiarthroplasty. b) Painful hemiarthroplasty with evidence of glenoid sclerosis and wear. c) Postoperative radiograph following revision with a cemented glenoid component with PEG and an uncemented stemmed humeral prosthesis.
- Lucency around glenoid component does not always corrolate with symptoms and may not be significant.
- Progression of lucency often is significant.
- Increased uptake on SPECT/CT is demonstrated Fig. 23.
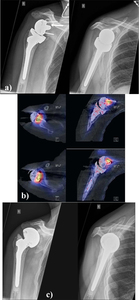
Fig. 23: a) AP and Y-view radiographs of the right shoulder showing wide radiolucent lines around the glenoid peg (white arrow) b) 99mTc-HDP-SPECT/CT showing increased tracer uptake at the glenoid component-host bone interface, which was interpreted as clear sign for mechanical loosening c) AP and Y-view radiographs of the right shoulder after revision to a bipolar cup prosthesis
References: http://www.internationalshoulderjournal.org
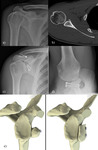
- Scapular notching - Seen in RTSA - Results when the medial aspect of the humeral cup contacts the lateral scapular margin. Fig. 32 Fig. 33 - -Can be caused from malpositioning of the implant,
and is shown to adversely affect clinical outcome.
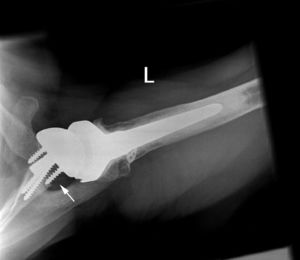
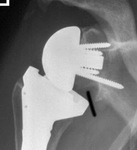
Fig. 33: Radiograph of a RTSA showing posterior notching resulting from impingement of the prosthesis in external rotation. Erosion of the posterior part of the scapula is seen as a radiolucency involving the posterior screw (white arrow)
References: http://jbjs.org
Infection
- More common with revisions.
- Seen as luceny around the implant and cortical thinning Fig. 36
- Can be managed by a 2-staged revision with a temporary cement spacer impregnated with antibiotics Fig. 35
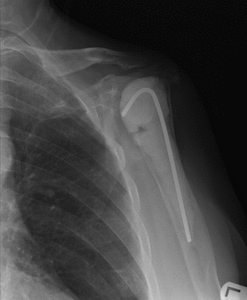
Fig. 35: AP radiograph of the left shoulder after implant removal for infection, demonstrating the placement of a cement spacer impregnated with antibiotics.
References: http://jbjs.org
Periprosthetic fracture Fig. 18
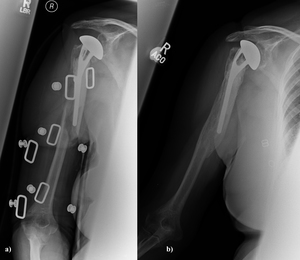
Fig. 18: a) spiral periprosthetic fracture around the stem (Type A). Metal artifact is from a humeral brace. b) demonstrates satisfactory bony union following non-operative treatment.
- Intraoperative 1% - greater risk with porous coated stems vs cemented
- Postoperative 0.5 - 2%
- Moer common in RA and women.
- Glenoid fractures are rare.
Classification (Wright and Cofield)
- Type - A fracture - centered at the tip of prosthesis with an extension of more than one-third of the length of the stem.
- Type - B fractures - centered at the tip but extension is less than one-third of the length of the stem.
- Type - C fractures are distal of the tip of the prosthesis.
NON ARTHROPLASTY METALWORK
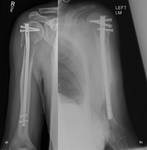
Intramedullary nail Fig. 27
- For fracture fixation - pathological and traumatic.
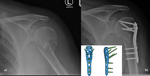
Plate fixation Fig. 28
- Multiple proximal holes with utilisation of locking screws.
This allows for a rigid construct and good for osteoporotic bone.
- Proximal Humeral Interlocking System - PHILOS - one brand
Bone anchors
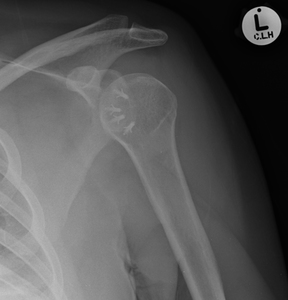
Fig. 29: Multiple metallic bone anchors situated within the proximal humerus (lesser tuberosity) following repair of the subscapularis tendon
Isolated screws Fig. 26
- Often away from site of injury.
- Used to anchor suture mateiral.
- Facilitate ligament reconstruction Fig. 25
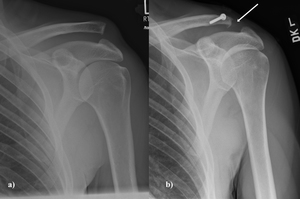
Fig. 25: a) A high grade ACJ dislocation (Grade V). b) a single cortical screw in the clavicle is used in the reconstruction of the coracoclavicular ligaments. There has been excision of the lateral end of the clavicle (white arrow)
- In cases of instability especially when there has been a failed Bankart reconstruction - coracoid transfer to reconstruct the anterior glenoid Fig. 31
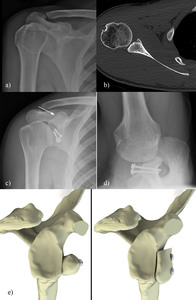
Fig. 31: a) Preoperative AP radiograph of a patient with anterior instability. b) Selected axial CT image shows a large bony Bankart. c,d) Post operative images following a Laterjet procedure. e) The procedure involves transfer of the coracoid with it's attached muscles to the deficient area over the front of the glenoid.
White arrow on c) demonstrates absent coracoid process.